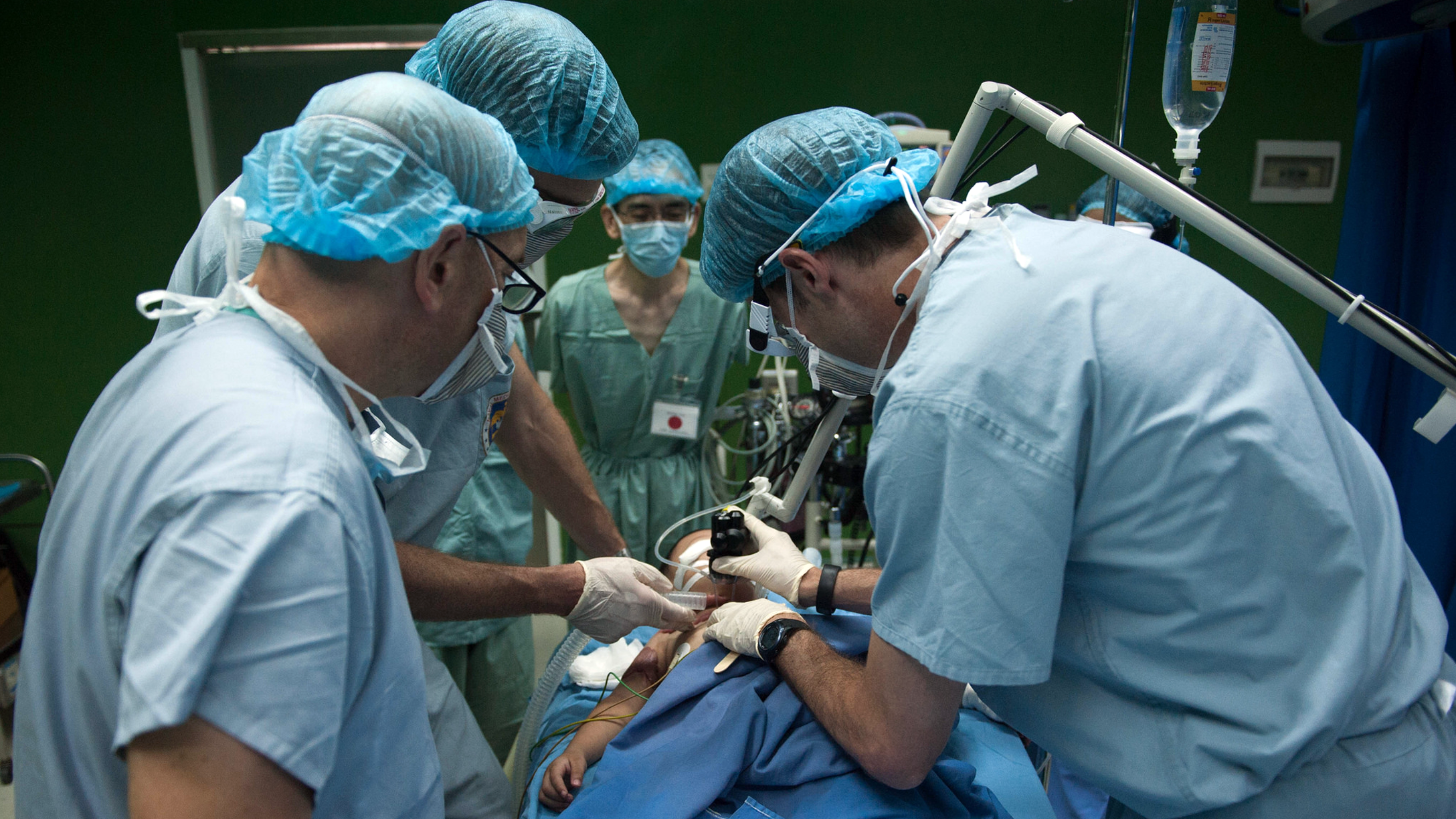
I spent nearly all my working life in hospitals. I was a doctor, an emergency medicine specialist actually. We could only practice in hospitals. Or perhaps do some retrieval in helicopters, but that wasn’t for me. So I ended up going in every working day to a hospital, to an emergency department full of sick people, often very sick people.
People who had sudden chest pain, or an arm that wouldn’t work, or were suddenly short of breath. These people surrounded me every working day. They usually had no choice. They called an ambulance, or their doctor said ‘You need to be in the hospital’, and off they went. I had a choice though. But I still kept coming.
And gradually, gradually, over 30 years, the pain, grief, hardship and outright misery got under my skin. Actually it got into my soul. It started to change me. I became increasingly fatalistic. I didn’t invest much of myself in too many things that mightn’t work out.
As an emergency physician, I started to change in other ways too. My rapid-fire, instant decision-making at work started to become a way of living outside of work. Times of quiet contemplation became less and less common. I felt I needed to be doing something most of the time. I didn’t mull things over, I just got on with it.
A workplace where everybody is carrying similar burdens has its drawbacks. In a crisis, and crises happen frequently in emergency, people don’t interact so much as bark at each other. I learnt to suppress my irritations and frustrations at not being able to control the way things went. My voice became quieter on the outside but louder on the inside.
To an external observer I was relaxed. Internally I filtered out everything that I didn’t need to attend to and just focused on a few key things. Alive or dead? Breathing or not? Circulation or not? I would immediately jump to the end of the process on first seeing a critically ill person and see the outcome. Should I invest too much or is this one too going to be futile?
The people I was looking after were of course negotiating their own particular mine fields. And not just their illnesses. Vulnerable, often frail, very sick and suddenly being forced to try to think of answers to a multitude of rapidly delivered questions. While the person in the next cubicle may have been screaming or dying. Some were too afraid to speak up when they should have.
And the risks they faced, not just from their illnesses, but from simply being there. The risk of not finding out in time what was about to kill them. The risk of finding something that was irrelevant but led the treating team down a rabbit hole of investigation that carried its own threats to life. The roulette wheel of harried clinical staff trying to figure out and remember doses and injections in too small a time window.
Then there were the moral dilemmas I faced on a daily basis. Not enough resources. So not enough staff, not enough room, not enough time. Having to assess people who were desperately ill in the waiting room because there was just no room. Because the hospital was full. Always full.
Strangely, perversely, I had a piece of luck. I got sick myself. Potentially very sick. I was diagnosed with multiple sclerosis.
While it took me a while to work out how to keep well, and much longer to work out that I needed to stop my crazy working life, the illness provided the circuit breaker. A decade or so after diagnosis I stopped seeing patients and started doing research exclusively. A few years later research into MS became my primary occupation.
My life is changing slowly. I can sit at work and think if I need to. I can sit at home and think if I need to. My life is slowing down. One day I hope to be going at the same pace as life is.
I realise now that my work was making me sick. Constant exposure, on a daily basis, to serious sickness and death, all in a pressure cooker environment, takes its toll. I feel drained just thinking about it. Emergency departments have to be there. Sudden illness or injury is all too common. Someone has to be there when it matters. But we need to work out what to do about those environments. And about the needs of the people within them, staff and patients alike.
Brighter minds than mine have grappled with these problems. But grapple we must if the next generation of emergency physicians is not to face the same problems. Not to mention their patients. Perhaps staffing these departments for the peaks, not the average, or worse still the troughs, as many departments seem to be. So when there is a real crisis and staff are reeling, they can exit the chaos. And perhaps talk to people good at listening. Or even go home. Take some time off. With others available to cover for them.
Perhaps we need to ask our patients how they would design their ideal emergency department. Has anyone thought to do that? I know they would like caring, kind, compassionate staff. Staff who are not carrying serious emotional damage with them to work and back every day. It would be good for all of us to get this right. And soon.
George Jelinek